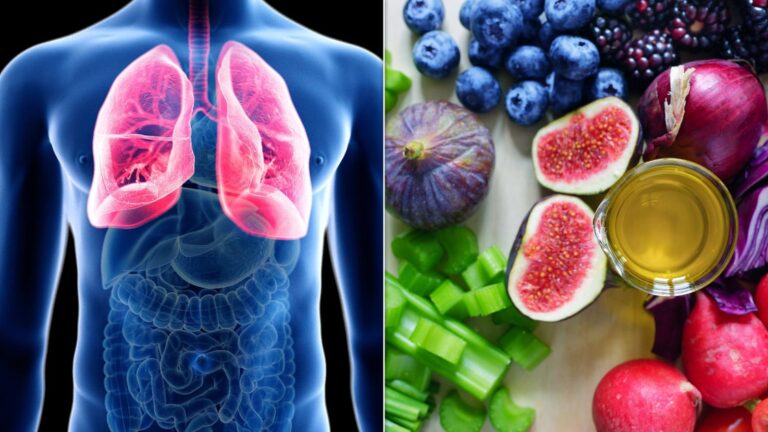
A new study conducted by the University of Southern California found that a group of 187 lung cancer patients under the age of 50, most of whom had never smoked, were found to have healthier-than-average diets — which raises concerns that there could be unexpected health risks with certain fruits, vegetables and grains.
The patients were also diagnosed with a form of lung cancer that is biologically different from the type associated with smoking.
What stood out among the group was that they had an average Healthy Eating Index (HEI) score of 65 out of 100, a high HEI compared to the national average of 57. Each patient ate more fruits, vegetables and whole grains than the average American adult, according to the study.
“Our research shows that younger non-smokers who eat a higher quantity of healthy foods than the general population are more likely to develop lung cancer,” Dr. Jorge Nieva, a medical oncologist and lung cancer specialist at USC Norris Comprehensive Cancer Center, and the lead investigator of the study, said in a statement. “These counter-intuitive findings raise important questions about an unknown environmental risk factor for lung cancer related to otherwise beneficial food that needs to be addressed.”
The study also found that, out of the patients in the study, women seemed to be diagnosed with lung cancer more often than men in their same age demographic, even though neither group smoked. The female patients reported consuming more fruits, vegetables and grains than the men.
There are several limitations with this research. For starters, the results only imply a correlation between a healthier diet and lung cancer in participants. There is no direct causation at this time. This was also a very small study; it’s not clear how this would apply to a broader population.
Dr. David Carbone, who contributed to the research, told HuffPost this has been an ongoing theory in the lung cancer field for years. Carbone, who is a member of the scientific advisory board at the Lung Cancer Foundation of America (LCFA) and a doctor at the Ohio State University Comprehensive Cancer Center, is a leading expert in lung cancer research and treatment.
“I’ve been in this business 30 or 40 years now, and I have noticed that it seems like our young patients with lung cancer seem to be the people who are objectively the healthiest,” Carbone said.
The study’s findings are just indicative that more research needs to go into these young people’s lung cancer cases — it does not mean certain fruits, vegetables and whole grains are poisonous.
“This is certainly not proof that eating these things causes lung cancer — that is way overextrapolation of the data,” he said. “This is association, not causation.”
One possible environmental culprit could be pesticides, given that fruits, vegetables and whole grains are exposed to higher pesticide levels than items like dairy or meat. Agricultural workers, who spray the pesticides before they plant the crops and again when the crops emerge, also have high rates of lung cancer.
But Carbone emphasizes pesticides aren’t definitive, either. For one, there hasn’t been a subset study examining lung cancer patients who were healthy and had organic-specific diets, where they exclusively ate produce grown without pesticides. Researchers also did not measure pesticide levels in the foods the patients were eating or in the patients themselves through blood or urine samples; instead, they worked with estimated pesticide exposure levels for the average fruit, vegetable and whole grain.
It was also a U.S.-based study, Carbone emphasized, and places like Europe have much stricter pesticide regulations, but are still diagnosing young non-smokers with lung cancer.
While some people think they’re protecting themselves from the potential threat of pesticides by washing their produce, Carbone noted that “a lot of these [pesticides] are — especially the insecticides — are designed to stick to the fruit and not wash off when it rains, so I’m not entirely sure how effective [washing the fruit] is.”
That then poses the question of whether fruits and vegetables that are peeled before eating — such as bananas and oranges — are less dangerous than, say, apples, Carbone said.
Carbone also pointed out that, in his experience, the patients who volunteer for clinical research projects usually have a healthier-than-average diet, which is why they feel comfortable getting involved and sharing personal information for studies. This could be unintentional selection bias, which skews toward health-conscious participants rather than the general population of young non-smokers with lung cancer.
“[The study] was exploratory, looking for signals, and this was one of the signals,” Carbone said about the patients’ healthy diets. “All of these things are hypotheses that probably should be tested.”